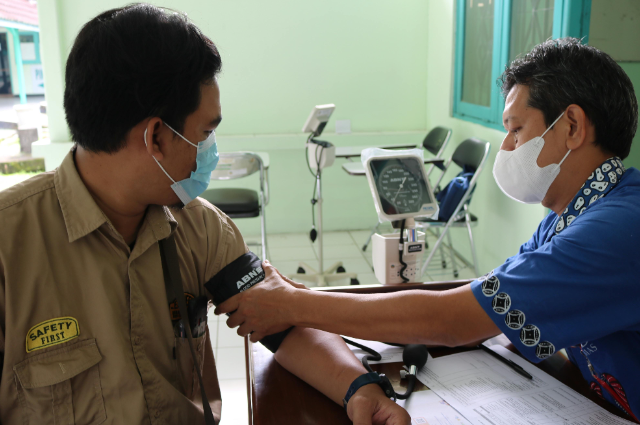
In the dense, underserved tribal belt of (Melghat) in Maharashtra, healthcare was once a distant privilege rather than a basic right. Marked by extreme poverty, malnutrition, and inaccessibility, the region struggled with some of the highest infant and maternal mortality rates in India. It was into this landscape that Dr Ravindra Kolhe and Dr Smita Kolhe stepped not merely as doctors but as architects of a sustainable, community-driven healthcare model that redefined rural service delivery.
Dr Ravindra Kolhe, deeply influenced by the philosophies of Mahatma Gandhi and Vinoba Bhave, envisioned a life rooted in service rather than urban success. After completing his MBBS, he consciously chose to work in Bairagarh, a remote village where even basic medical infrastructure was absent. His preparation was unconventional yet practical; he trained himself to diagnose and treat illnesses without reliance on advanced tools, inspired by the globally recognised rural healthcare manual Where There Is No Doctor by David Werner. This approach would later prove crucial in a setting where electricity, let alone X-rays, was inconsistent.
However, the success of this mission cannot be understood without acknowledging the role of Dr Smita Kolhe. A practitioner of [Ayurveda and Homoeopathy], she entered this life with full awareness of its challenges. Their marriage itself symbolised a radical departure from societal norms, grounded in shared purpose rather than comfort. Her decision to treat their critically ill newborn within the same limited conditions as the villagers marked a turning point. It dissolved the invisible barrier between “doctor” and “patient,” embedding trust at the heart of their work.
(The Kolhes)’ The contribution to healthcare in Melghat is measurable and profound. [Studies and regional reports indicate that infant mortality rates in their working area dropped from nearly 200 per 1,000 live births to around 40, while pre-school mortality rates saw a similar decline]. These improvements were not achieved through high-cost interventions but through low-cost, high-impact strategies, timely diagnosis, community awareness, and accessible treatment.
- By charging a nominal fee of 1 to 2rs, they ensured that healthcare remained inclusive, while simultaneously preserving the dignity of those seeking treatment. What makes their work particularly significant in the context of public health is their understanding of disease as a socio-economic outcome rather than a purely biological condition. As Dr Ravindra Kolhe observed, illnesses like pneumonia and malnutrition were not isolated medical issues but
- Symptoms of deeper structural problems: lack of clothing, seasonal unemployment, and food insecurity. This insight aligns with broader frameworks in Public Health, which emphasise social determinants of health as critical drivers of disease patterns. Acting on this understanding, the Kolhes expanded their work beyond clinical care into livelihood generation and agricultural reform. They introduced fungus-resistant seed varieties, encouraged sustainable farming practices, and [conducted training sessions to educate villagers about government schemes]. These interventions gradually reduced economic vulnerability, which in turn had a direct positive impact on health outcomes.
- In effect, they created a holistic development model where healthcare, nutrition, and livelihood were interconnected rather than treated as separate domains. Infrastructure development also played a crucial role in transforming the region. When offered personal benefits by political leaders such as Nitin Gadkari, the Kolhis chose to advocate for public goods instead—roads, electricity, and healthcare centres. Today, Melghat has significantly improved connectivity and multiple primary health centres, demonstrating how grassroots advocacy can influence policy-level decisions.
Their work also offers a compelling case study in community integration. Unlike many external interventions that fail due to a lack of cultural understanding, the Kolhes immersed themselves in the local way of life.] They adopted the community’s lifestyle, participated in its challenges, and earned trust through shared experience rather than authority. This approach resonates with participatory models of development, where communities are not passive recipients but active stakeholders in their own progress.
Recognition for their efforts came in the form of the Padma Shri in 2019, one of India’s highest civilian honours. They were also featured on Kaun Banega Crorepati, bringing national attention to their work.
However, the true measure of their success lies not in awards, but in the lives of the children who survived, the families who gained stability, and the community that moved from despair to resilience. From a policy perspective, the Kolhes’ model raises important questions about scalability and replication. Can such deeply personalised, community-driven interventions be expanded across other underserved regions? While the uniqueness of their commitment may be difficult to replicate, the principles underlying their work—affordability, accessibility, community trust, and focus on root causes—offer valuable insights for designing effective rural healthcare systems.
In conclusion, the story of Dr Ravindra and Dr Smita Kolhe is not just an inspiring narrative but a practical blueprint for sustainable development. It challenges conventional notions of healthcare by demonstrating that meaningful change does not always require advanced technology or large-scale funding. Sometimes, it begins with a simple yet radical decision to stay, to serve, and to see people not as patients, but as equals.
References
